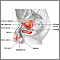
A cystometric study measures the amount of fluid in the bladder when you first feel the need to urinate, when you are able to sense fullness, and when your bladder is completely full.
How the Test is Performed
Prior to the cystometric study, you may be asked to urinate (void) into a special container that is interfaced with a computer. This type of study is called a uroflow, during which the following will be recorded by the computer:
- The time it takes you to begin urinating
- The pattern, speed, and continuity of your urinary stream
- The amount of urine
- How long it took you to empty your bladder
You will then lie down, and a thin, flexible tube (catheter) is gently placed in your bladder. The catheter measures any urine left in the bladder. A smaller catheter is sometimes placed in your rectum in order to measure abdominal pressure. Measuring electrodes, similar to the sticky pads used for an ECG, are placed near the rectum.
A tube used to monitor bladder pressure (cystometer) is attached to the catheter. Water flows into the bladder at a controlled rate. You will be asked to tell your health care provider when you first feel the need to urinate and when you feel that your bladder is completely full.
Often, your provider may need more information and will order tests to evaluate your bladder function. This set of tests is often referred to as urodynamics or complete urodynamics. The combination includes three tests:
- Measured voiding without a catheter (uroflow)
- Cystometry (filling phase)
- Voiding or emptying phase test
For complete urodynamic testing, a much smaller catheter is placed in the bladder. You will be able to urinate around it. Because this special catheter has a sensor on the tip, the computer can measure the pressure and volumes as your bladder fills and as you empty it. You may be asked to cough or push so that the provider can check for urine leakage. This type of complete testing can reveal a lot of information about your bladder function.
For even more information, x-rays can be taken during the test. In this case, instead of water, a special fluid (contrast) that shows on an x-ray is used to fill your bladder. This type of urodynamics is called videourodynamics.
How to Prepare for the Test
No special preparations are needed for this test.
For infants and children, preparation depends on the child's age, past experiences, and level of trust. For general information regarding how you can prepare your child, see the following topics:
- Preschooler test or procedure preparation (3 to 6 years)
- School age test or procedure preparation (6 to 12 years)
- Adolescent test or procedure preparation (12 to 18 years)
How the Test will Feel
There is some discomfort associated with this test. You may experience:
- Bladder filling
- Flushing
- Nausea
- Pain
- Sweating
- Urgent need to urinate
- Burning
Why the Test is Performed
The test will help determine the cause of bladder voiding (emptying) dysfunction.
Normal Results
Normal results vary and should be discussed with your provider.
What Abnormal Results Mean
Abnormal results may be due to:
- Overactive bladder
- Reduced bladder capacity
Risks
There is a slight risk for urinary tract infection and blood in the urine.
Considerations
This test should not be done if you have a known urinary tract infection. Existing infection increases the possibility of false test results. The test itself increases the possibility of spreading the infection.
Alternative Names
CMG; Cystometrogram
Images
References
Brucker BM, Nitti VW. Urodynamic and video-urodynamic evaluation of the lower urinary tract. In: Partin AW, Dmochowski RR, Kavoussi LR, Peters CA, eds. Campbell-Walsh-Wein Urology. 12th ed. Philadelphia, PA: Elsevier; 2021:chap 114.
Grochmal SA. Office testing and treatment options for interstitial cystitic (painful bladder syndrome). In: Fowler GC, ed. Pfenninger and Fowler's Procedures for Primary Care. 4th ed. Philadelphia, PA: Elsevier; 2020:chap 98.
Lentz GM, Miller JL. Lower urinary tract function and disorders: physiology of micturition, voiding dysfunction, urinary incontinence, urinary tract infections, and painful bladder syndrome. In: Gershenson DM, Lentz GM, Valea FA, Lobo RA, eds. Comprehensive Gynecology. 8th ed. Philadelphia, PA: Elsevier; 2022:chap 21.
Review Date 10/15/2023
Updated by: Kelly L. Stratton, MD, FACS, Associate Professor, Department of Urology, University of Oklahoma Health Sciences Center, Oklahoma City, OK. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.