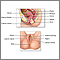
Cervix cryosurgery is a procedure to freeze and destroy abnormal tissue in the cervix.
Description
Cryotherapy is done in the health care provider's office while you are awake. You may have slight cramping. You may have some amount of pain during the surgery.
To perform the procedure:
- An instrument is inserted into the vagina to hold the walls open so that the doctor can see the cervix.
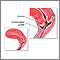
- The doctor then inserts a device called a cryoprobe into the vagina. The device is placed firmly on the surface of the cervix, covering the abnormal tissue.
- Compressed nitrogen gas flows through the instrument, making the metal cold enough to freeze and destroy the tissue.
An "ice ball" forms on the cervix, killing the abnormal cells. For the treatment to be most effective:
- The freezing is done for 3 minutes
- The cervix is allowed to thaw for 5 minutes
- Freezing is repeated for another 3 minutes
Why the Procedure is Performed
This procedure may be done to:
- Treat cervicitis
- Treat cervical dysplasia
Your provider will help you to decide if cryosurgery is right for your condition.
Risks
Risks of any surgery are:
- Bleeding
- Infection
Cryosurgery may cause scarring of the cervix, but most of the time, it is very minor. More severe scarring may make it more difficult to get pregnant, or cause increased cramping with menstrual periods.
Before the Procedure
Your provider may suggest you to take medicine such as ibuprofen 1 hour before the procedure. This may reduce pain during the procedure.
After the Procedure
You might feel lightheaded right after the procedure. If this happens, lie down flat on the examination table so that you do not faint. This feeling should go away in a few minutes.
You can resume almost all of your normal activities right after surgery.
For 2 to 3 weeks after the surgery, you will have a lot of watery discharge caused by the shedding (sloughing) of the dead cervical tissue.
You may need to avoid sexual intercourse and using tampons for several weeks.
Avoid douching. This can cause severe infections in the uterus and tubes.
Alternative Names
Cervix surgery; Cryosurgery - female; Cervical dysplasia - cryosurgery
References
Lewis MR, Pfenninger JL. Cryotherapy of the cervix. In: Fowler GC, ed. Pfenninger and Fowler's Procedures for Primary Care. 4th ed. Philadelphia, PA: Elsevier; 2020:chap 125.
Nayar R, Chhieng DC, Crothers B, et al. Moving forward-the 2019 ASCCP risk-based management consensus guidelines for abnormal cervical cancer screening tests and cancer precursors and beyond: implications and suggestions for laboratories. J Am Soc Cytopathol. 2020;9(4):291-303. Erratum in: J Am Soc Cytopathol. 2020. PMID: 32565297 pubmed.ncbi.nlm.nih.gov/32565297/.
Salcedo MP, Phoolcharoen N, Schmeler KM. Intraepithelial neoplasia of the lower genital tract (cervix, vagina, vulva): etiology, screening, diagnosis, management. In: Gershenson DM, Lentz GM, Valea FA, Lobo RA, eds. Comprehensive Gynecology. 8th ed. Philadelphia, PA: Elsevier; 2022: chap 29.
Review Date 1/10/2022
Updated by: John D. Jacobson, MD, Department of Obstetrics and Gynecology, Loma Linda University School of Medicine, Loma Linda, CA. Also reviewed by David Zieve, MD, MHA, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.