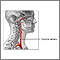
Giant cell arteritis (GCA) is inflammation and damage to the blood vessels that supply blood to the head, neck, upper body and arms. It is also called temporal arteritis.
Causes
Giant cell arteritis affects medium-to-large arteries. It causes inflammation, swelling, tenderness, and damage to the blood vessels that supply blood to the head, neck, upper body, and arms. It most commonly occurs in the arteries around the temples (temporal arteries). These arteries branch off from the carotid artery in the neck. In some cases, the condition can occur in medium-to-large arteries in other places in the body as well.
The cause of the condition is unknown. It is believed to be due in part to a faulty immune response. The disorder has been linked to some infections and to certain genes.
Giant cell arteritis is more common in people with another inflammatory disorder known as polymyalgia rheumatica. While GCA is a considerably uncommon condition, it primarily affects individuals over the age of 50. It is most common in people of northern European descent. The condition may run in families.
Symptoms
Some common symptoms of this problem are:
- New throbbing headache on one side of the head or the back of the head
- Tenderness when touching the scalp
Other symptoms may include:
- Jaw pain that occurs when chewing (called jaw claudication)
- Pain in the arm after using it
- Muscle aches
- Pain and stiffness in the neck, upper arms, shoulder, and hips (polymyalgia rheumatica)
- Weakness, excessive tiredness
- Fever
- General ill feeling
Problems with eyesight may occur, and at times may begin suddenly. These problems include:
- Blurred vision
- Double vision
- Sudden reduced vision (blindness in one or both eyes)
Exams and Tests
The health care provider will examine your head.
- The scalp is often sensitive to touch.
- There may be a tender, thick artery on one side of the head, most often over one or both temples.
Blood tests may include:
- Hemoglobin or hematocrit
- Liver function tests
- Sedimentation rate (ESR) and C-reactive protein (CRP)
Blood tests alone cannot provide a diagnosis. You will need to have a biopsy of the temporal artery. This is a surgical procedure that can be done as an outpatient.
You may also have other tests, including:
- Color Doppler ultrasound of the temporal arteries. This may take the place of a temporal artery biopsy if done by someone experienced with the procedure.
- MRI or CT angiography.
- PET scan.
- Biopsy. If the ultrasound is positive a biopsy may not be needed. If the ultrasound is negative, the heath care provider will decide if a biopsy is needed.
Treatment
Getting prompt treatment can help prevent severe problems such as blindness or stroke.
When giant cell arteritis is suspected, you will receive corticosteroids, such as prednisone, by mouth. These medicines are often started even before a biopsy is done. You may also be told to take aspirin.
Most people begin to feel better within a few days after starting treatment. The dose of corticosteroids will be cut back very slowly. However, you will need to take medicine for 1 to 2 years.
If the diagnosis of giant cell arteritis is made, in most people a biologic medicine called tocilizumab will be added. This medicine reduces the amount of corticosteroids needed to control the disease.
Long-term treatment with corticosteroids can make bones thinner and increase your chance of a fracture. You will need to take the following steps to protect your bone strength.
- Avoid smoking and excess alcohol intake.
- Take extra calcium and vitamin D (based on your provider's advice).
- Start walking or other forms of weight-bearing exercises.
- Have your bones checked with a bone mineral density (BMD) test or DEXA scan.
- Take a bisphosphonate medicine, such as alendronate (Fosamax), as prescribed by your provider.
Outlook (Prognosis)
Most people make a full recovery, but treatment may be needed for 1 to 2 years or longer. The condition may return at a later date.
Damage to other blood vessels in the body, such as aneurysms (ballooning of the blood vessels), may occur. This damage can lead to a stroke in the future.
When to Contact a Medical Professional
Contact your provider if you have:
- Throbbing headache that does not go away
- Loss of vision
- Other symptoms of temporal arteritis
You may be referred to a specialist who treats temporal arteritis.
Prevention
There is no known prevention.
Alternative Names
Arteritis - temporal; Cranial arteritis; GCA
Images
References
Dejaco C, Ramiro S, Duftner C, et al. EULAR recommendations for the use of imaging in large vessel vasculitis in clinical practice. Ann Rheum Dis. 2018;77(5):636-643. PMID: 29358285 pubmed.ncbi.nlm.nih.gov/29358285/.
Hellmann DB. Giant cell arteritis, polymyalgia rheumatica, and Takayasu's arteritis. In: Firestein GS, Budd RC, Gabriel SE, Koretzky GA, McInnes IB, O'Dell JR, eds. Firestein & Kelley's Textbook of Rheumatology. 11th ed. Philadelphia, PA: Elsevier; 2021:chap 93.
James WD, Elston DM, Treat JR, Rosenbach MA, Neuhaus IM. Cutaneous vascular diseases. In: James WD, Elston DM, Treat JR, Rosenbach MA, Neuhaus IM, eds. Andrews' Diseases of the Skin: Clinical Dermatology. 13th ed. Philadelphia, PA: Elsevier; 2020:chap 35.
Koster MJ, Matteson EL, Warrington KJ. Large-vessel giant cell arteritis: diagnosis, monitoring and management. Rheumatology (Oxford). 2018;57(suppl_2):ii32-ii42. PMID: 29982778 pubmed.ncbi.nlm.nih.gov/29982778/.
Matza MA, Unizony SH. Polymyalgia rheumatica and giant cell arteritis. In: Kellerman RD, Rakel DP, Heidelbaugh JJ, Lee EM, eds. Conn's Current Therapy 2024. Philadelphia, PA: Elsevier; 2024:1037-1039.
Stone JH, Tuckwell K, Dimonaco S, et al. Trial of tocilizumab in giant-cell arteritis. N Engl J Med. 2017;377(4):317-328. PMID: 28745999 pubmed.ncbi.nlm.nih.gov/28745999/.
Tamaki H, Hajj-Ali RA. Tocilizumab for giant cell arteritis - a new giant step in an old disease. JAMA Neurol. 2018;75(2):145-146. PMID: 29255889 pubmed.ncbi.nlm.nih.gov/29255889/.
Review Date 1/25/2023
Updated by: Neil J. Gonter, MD, Assistant Professor of Medicine, Columbia University, NY and private practice specializing in Rheumatology at Rheumatology Associates of North Jersey, Teaneck, NJ. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team. Editorial update 03/08/2024.