Human immunodeficiency virus (HIV) is the virus that causes acquired immunodeficiency syndrome (AIDS). When a person becomes infected with HIV, the virus attacks and weakens the immune system. As the immune system weakens, the person is at risk for getting life-threatening infections and cancers. When that happens, the illness is called AIDS. Once a person has the virus, it stays inside the body for life.
Causes
The virus is spread (transmitted) person-to-person through certain body fluids:
- Blood
- Semen and preseminal fluid
- Rectal fluids
- Vaginal fluids
- Breast milk
HIV can be spread if these fluids come in contact with:
- Mucous membranes (inside of the mouth, penis, vagina, rectum)
- Damaged tissue (tissue that has been cut or scraped)
- The blood stream by injection
HIV cannot be spread through sweat, saliva, or urine.
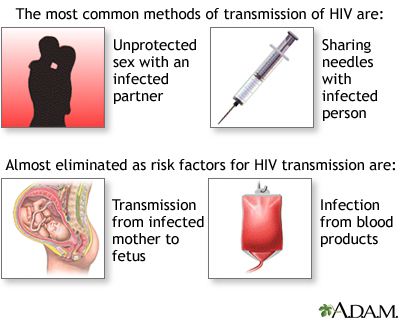
In the United States, HIV is mainly spread:
- Through vaginal or anal sex without using a condom with someone who has HIV who is not taking medicines to prevent or treat HIV
- Through needle sharing or other equipment used to inject drugs with someone who has HIV
Less often, HIV is spread:
- From mother to child. A pregnant woman can spread the virus to her fetus through their shared blood circulation, or a nursing mother can pass it to her baby through her breast milk. Testing and treatment of HIV-positive mothers has helped lower the number of babies getting HIV.
- Through needle sticks or other sharp objects that are contaminated with HIV (mainly health care workers).
The virus is NOT spread by:
- Casual contact, such as hugging or closed-mouth kissing
- Mosquitoes or pets
- Participating in sports
- Touching items that were touched by a person infected with the virus
- Eating food handled by a person with HIV
- Intimate contact with an HIV-positive person with a stably undetectable viral load
HIV and blood or organ donation:
- HIV is not spread to a person who donates blood or organs. People who donate organs are never in direct contact with the people who receive them. Likewise, a person who donates blood is never in contact with the person receiving it. In all of these procedures, sterile needles and instruments are used.
- Blood banks and organ donor programs thoroughly check (screen) donors, blood, and tissues. It is very unlikely to get HIV from blood transfusions, blood products, or organ or tissue transplants.
Risk factors for getting HIV include:
- Having unprotected anal or vaginal sex. Receptive anal sex is the riskiest. Having multiple partners also increases the risk. Using a new condom correctly every time you have sex greatly helps lower this risk.
- Using drugs and sharing needles or syringes.
- Having a sexual partner with HIV who is not taking HIV medicines or who has a detectable viral load.
- Having a sexually-transmitted disease (STD).
Symptoms
Symptoms related to acute HIV infection (when a person is first infected) can be similar to the flu or other viral illnesses. They include:
- Fever and muscle pains
- Headache
- Sore throat
- Night sweats
- Mouth sores, including yeast infection (thrush)
- Swollen lymph glands
- Diarrhea
Many people have no symptoms when they are first infected with HIV.
Acute HIV infection (Stage 1) progresses over a few weeks to months to become chronic or asymptomatic HIV infection (Stage 2) (no symptoms). This stage can last 10 years or longer. During this period, the person might have no reason to suspect they have HIV, but they can spread the virus to others.
If they are not treated, almost all people infected with HIV will develop AIDS (Stage 3). Some people develop AIDS within a few years of infection. Others remain completely healthy after 10 or even 20 years (called long-term nonprogressors).
People with AIDS have had their immune system damaged by HIV. They are at very high risk of getting infections that are uncommon in people with a healthy immune system. These infections are called opportunistic infections and can affect any part of the body. These can be caused by:
- Bacteria
- Viruses
- Fungi
- Protozoa
People with AIDS are also at higher risk for certain cancers, especially lymphomas and a skin cancer called Kaposi sarcoma.
Symptoms depend on the particular infection and which part of the body is infected.
Lung infections are common in AIDS and often cause cough, fever, and shortness of breath.
Intestinal infections are also common and can cause:
- Diarrhea
- Abdominal pain
- Vomiting
- Swallowing problems
Other common symptoms in people with HIV infection and AIDS include:
- Weight loss
- Fever
- Sweats
- Rashes
- Swollen lymph glands
Exams and Tests
There are tests that are done to check if you've been infected with HIV.
DIAGNOSTIC TESTS
In general, testing is a 2-step process:
- Screening test -- There are several kinds of tests. Some are blood tests, others are mouth fluid tests. They check for antibodies to the HIV virus, HIV antigen, or both. Some screening tests can give results in 30 minutes or less.
- Follow-up test -- This is also called a confirmatory test. It is often done when the screening test is positive.
Home tests are available to test for HIV. If you plan to use one, check to make sure it is approved by the FDA. Follow instructions on the packaging to ensure the results are as accurate as possible.
The Centers for Disease Control and Prevention (CDC) recommends that everyone ages 15 to 65 have a screening test for HIV. People with risky behaviors should be tested regularly. Pregnant women should also have a screening test.
TESTS AFTER BEING DIAGNOSED WITH HIV
People with AIDS should have regular blood tests to check their CD4 cell count:
- CD4 T cells are the blood cells that HIV attacks. They are also called T4 cells or "helper T cells."
- As HIV damages the immune system, the CD4 count drops. A normal CD4 count is from 500 to 1,500 cells/mm3 of blood.
- People usually develop symptoms when their CD4 count drops below 350. More serious complications occur when the CD4 count drops to 200. When the count is below 200, the person is said to have AIDS.
Other tests include:
- HIV RNA level, or viral load, to check how much HIV is in the blood
- A resistance test to see if the virus has any changes in the genetic code that would lead to resistance to the medicines used to treat HIV
- Complete blood count, blood chemistry, and urine test
- Tests for other sexually transmitted infections
- TB test
- Pap test to check for cervical cancer
- Anal Pap test to check for cancer of the anus
Treatment
HIV/AIDS is treated with medicines that stop the virus from multiplying. This treatment is called antiretroviral therapy (ART).
In the past, people with HIV infection would start antiretroviral treatment after their CD4 count dropped or they developed HIV complications. Today, HIV treatment is recommended for all people with HIV infection, even if their CD4 count is still normal.
There are two types or treatment:
- Pills are given to people who are just starting treatment.
- Shots may be given to people who have an undetectable viral load or who have been virally suppressed for at least 3 months. Shots may be given every month or every other month.
Regular blood tests are needed to make sure the virus level in the blood (viral load) is kept low or suppressed. The goal of treatment is to lower the HIV virus in the blood to a level that is so low that the test can't detect it. This is called an undetectable viral load.
If the CD4 count already dropped before treatment was started, it will usually slowly go up. HIV complications often disappear as the immune system recovers.
Support Groups
Joining a support group where members share common experiences and problems can often help lower the emotional stress of having a long-term illness.
Outlook (Prognosis)
With treatment, most people with HIV/AIDS can live a healthy and normal life.
Current treatments do not cure the infection. The medicines only work as long as they are taken every day. If the medicines are stopped, the viral load will go up and the CD4 count will drop. If the medicines are not taken regularly, the virus can become resistant to one or more of the medicines, and the treatment will stop working.
People who are on treatment need to see their health care providers regularly. This is to make sure the medicines are working and to check for side effects of the medicines.
When to Contact a Medical Professional
Contact your provider for an appointment if you have any risk factors for HIV infection. Also contact your provider if you develop symptoms of AIDS. By law, the results of HIV testing must be kept confidential (private). Your provider will review your test results with you.
Prevention
Preventing HIV/AIDS:
- Get tested. People who don't know they have HIV infection and who look and feel healthy are the most likely to transmit it to others.
- Do not use illegal drugs and do not share needles or syringes. Many communities have needle exchange programs where you can get rid of used syringes and get new, sterile ones. Staff at these programs can also refer you for addiction treatment.
- Avoid contact with another person's blood. If possible, wear protective clothing, a mask, and goggles when caring for people who are injured.
- If you test positive for HIV, you can pass the virus to others. You should not donate blood, plasma, body organs, or sperm.
- HIV-positive women who might become pregnant should talk to their provider about the risk to their unborn child. They should also discuss methods to prevent their baby from becoming infected, such as taking antiretroviral medicines during pregnancy.
- Breastfeeding should be avoided to prevent passing HIV to infants through breast milk.
Safer sex practices, such as using latex condoms, are effective in preventing the spread of HIV. But there is still a risk of getting the infection, even with the use of condoms (for example, condoms can tear).
In people who aren't infected with the virus, but are at high risk of getting it, certain medicines can help prevent infection.
- Truvada (emtricitabine and tenofovir disoproxil fumarate) - taken as a pill
- Descovy (emtricitabine and tenofovir alafenamide) - taken as a pill
- Apretude (cabotegravir) - given as a shot every other month to help prevent infection
This treatment is known as pre-exposure prophylaxis, or PrEP. Talk to your provider if you think PrEP might be right for you.
HIV-positive people who are taking antiretroviral medicines and have no detectible virus in their blood do not transmit the virus.
The US blood supply is among the safest in the world. Nearly all people infected with HIV through blood transfusions received those transfusions before 1985, the year HIV testing began for all donated blood.
If you believe you have been exposed to HIV, seek medical attention right away. Do not delay. Starting antiviral medicines right after the exposure (up to 3 days after) can reduce the chance that you will be infected. This is called post-exposure prophylaxis (PEP). It has been used to prevent transmission in health care workers injured by needlesticks.
Alternative Names
HIV infection; Infection - HIV; Human immunodeficiency virus; Acquired immune deficiency syndrome: HIV-1
Images
 STDs and ecological niches
STDs and ecological niches HIV
HIV Primary HIV infection
Primary HIV infection Canker sore (aphthous ulcer)
Canker sore (aphthous ulcer)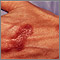 Mycobacterium marinum infection on the hand
Mycobacterium marinum infection on the hand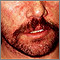 Dermatitis - seborrheic on the face
Dermatitis - seborrheic on the face AIDS
AIDS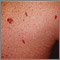 Kaposi sarcoma - close-up
Kaposi sarcoma - close-up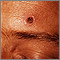 Histoplasmosis, disseminated in HIV patient
Histoplasmosis, disseminated in HIV patient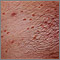 Molluscum on the chest
Molluscum on the chest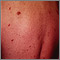 Kaposi sarcoma on the back
Kaposi sarcoma on the back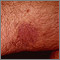 Kaposi's sarcoma on the thigh
Kaposi's sarcoma on the thigh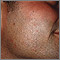 Molluscum contagiosum on the face
Molluscum contagiosum on the face Antibodies
Antibodies Tuberculosis in the lung
Tuberculosis in the lung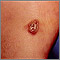 Kaposi sarcoma - lesion on the foot
Kaposi sarcoma - lesion on the foot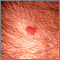 Kaposi sarcoma - perianal
Kaposi sarcoma - perianal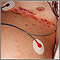 Herpes zoster (shingles) disseminated
Herpes zoster (shingles) disseminated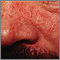 Dermatitis seborrheic - close-up
Dermatitis seborrheic - close-up
References
Centers for Disease Control and Prevention website. About HIV. www.cdc.gov/hiv/basics/whatishiv.html. Reviewed June 30, 2022. Accessed June 2, 2023.
Centers for Disease Control and Prevention website. PrEP (pre-exposure prophylaxis). www.cdc.gov/hiv/basics/prep.html. Reviewed June 3, 2022. Accessed June 2, 2023.
DiNenno EA, Prejean J, Irwin K, et al. Recommendations for HIV screening of gay, bisexual, and other men who have sex with men - United States, 2017. MMWR Morb Mortal Wkly Rep. 2017;66(31):830-832. www.cdc.gov/mmwr/volumes/66/wr/mm6631a3.htm.
Reitz MS, Gallo RC. Human immunodeficiency viruses. In: Bennett JE, Dolin R, Blaser MJ, eds. Mandell, Douglas, and Bennett's Principles and Practice of Infectious Diseases. 9th ed. Philadelphia, PA: Elsevier; 2020:chap 169.
Simonetti F, Dewar R, Maldarelli F. Diagnosis of human immunodeficiency virus infection. In: Bennett JE, Dolin R, Blaser MJ, eds. Mandell, Douglas, and Bennett's Principles and Practice of Infectious Diseases. 9th ed. Philadelphia, PA: Elsevier; 2020:chap 120.
Tsibris AMN, Hirsch MS. Antiretroviral therapy for human immunodeficiency virus infection. In: Goldman L, Cooney KA, eds. Goldman-Cecil Medicine. 27th ed. Philadelphia, PA: Elsevier; 2024:chap 128.
US Department of Health and Human Services, Clinical Info.gov website. Guidelines for the use of antiretroviral agents in adults and adolescents with HIV. clinicalinfo.hiv.gov/en/guidelines/hiv-clinical-guidelines-adult-and-adolescent-arv/whats-new?view=full. Updated March 23, 2023. Accessed June 2, 2023.
US Preventive Services Task Force, Owens DK, Davidson KW, Krist AH, et al. Screening for HIV Infection: US Preventive Services Task Force Recommendation Statement. JAMA. 2019;321(23):2326-2336. PMID: 31184701 pubmed.ncbi.nlm.nih.gov/31184701/.
Verma A, Berger JR. Neurological manifestations of human immunodeficiency virus infection in adults. In: Jankovic J, Mazziotta JC, Pomeroy SL, Newman NJ, eds. Bradley and Daroff's Neurology in Clinical Practice. 8th ed. Philadelphia, PA: Elsevier; 2022:chap 77.
Review Date 5/19/2023
Updated by: Jatin M. Vyas, MD, PhD, Associate Professor in Medicine, Harvard Medical School; Associate in Medicine, Division of Infectious Disease, Department of Medicine, Massachusetts General Hospital, Boston, MA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.





















