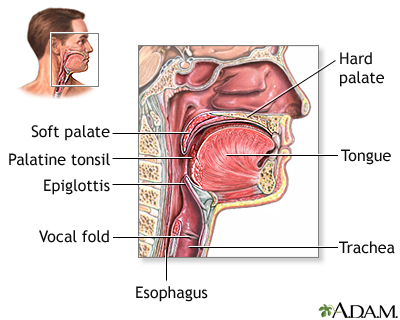
Strep throat is a disease that causes a sore throat (pharyngitis). It is an infection with a bacteria called group A streptococcus.
Causes
Strep throat is most common in children from ages 5 and 15, although anyone can get it.
Strep throat is spread by person-to-person contact with fluids from the nose or saliva. It commonly spreads among family or household members.
Symptoms
Symptoms appear about 2 to 5 days after coming in contact with the strep germ. They may be mild or severe.
Common symptoms include:
- Fever that may begin suddenly and is often the highest on the second day
- Chills
- Red, sore throat that may have white patches
- Pain when swallowing
- Swollen, tender neck glands
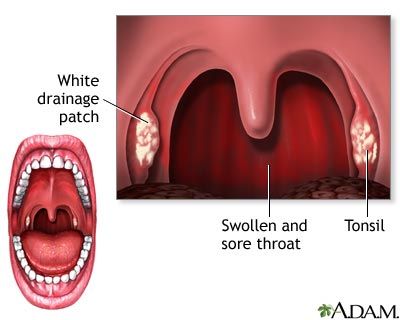
Other symptoms may include:
- General ill feeling
- A loss of appetite and abnormal sense of taste
- Headache
- Nausea
Some strains of strep throat can lead to a scarlet fever-like rash. The rash first appears on the neck and chest. It may then spread over the body. The rash may feel rough like sandpaper.
The same germ that causes strep throat may also cause symptoms of a sinus infection or an ear infection.
Exams and Tests
Many other causes of sore throat may have the same symptoms. Your health care provider must do a test to diagnose strep throat and decide whether to prescribe antibiotics.
A rapid strep test can be done in most provider offices. However, the test may be negative, even if strep is present.
If the rapid strep test is negative and your provider still suspects that the strep bacteria is causing the sore throat, a throat swab can be tested (cultured) to see if strep grows from it. Results will take 1 to 2 days.
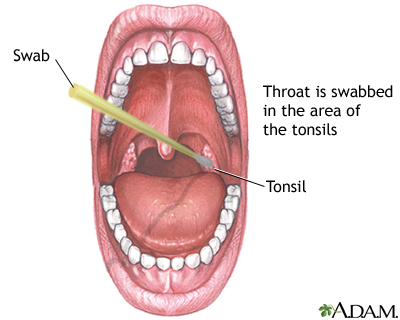
Treatment
Most sore throats are caused by viruses, not bacteria.
A sore throat should be treated with antibiotics only if the strep test is positive. Antibiotics are taken to speed up your recovery and to prevent rare but more serious health problems, such as rheumatic fever.
Penicillin or amoxicillin are most often the first drugs to be tried.
- Certain other antibiotics may also work against the strep bacteria.
- Antibiotics should be taken for 10 days, even though symptoms are often gone within a few days.
The following tips may help your sore throat feel better:
- Drink warm liquids, such as lemon tea or tea with honey.
- Gargle several times a day with warm salt water (1/2 tsp or 3 grams of salt in 1 cup or 240 milliliters water).
- Drink cold liquids or suck on fruit-flavored ice pops.
- Suck on hard candies or throat lozenges. Young children should not be given these products because they can choke on them.
- A cool-mist vaporizer or humidifier can moisten and soothe a dry and painful throat.
- Try over-the-counter pain medicines, such as acetaminophen (Tylenol) or ibuprofen (Advil, Motrin).
Outlook (Prognosis)
Symptoms of strep throat most often get better in about 1 week. Untreated, strep can lead to serious complications.
Possible Complications
Complications may include:
- Kidney disease caused by strep
- A skin condition in which small, red, and scaly teardrop-shaped spots appear on the arms, legs, and middle of the body, called guttate psoriasis
- Abscess in the area around the tonsils
- Rheumatic fever
- Scarlet fever
When to Contact a Medical Professional
Contact your provider if you or your child develops the symptoms of strep throat. Also, contact your provider if symptoms do not get better within 24 to 48 hours of starting treatment.
Prevention
Most people with strep can spread the infection to others until they have been on antibiotics for 24 to 48 hours. They should stay home from school, daycare, or work until they have been on antibiotics for at least a day.
Get a new toothbrush after 2 or 3 days, but before finishing the antibiotics. Otherwise, the bacteria can live on the toothbrush and reinfect you when the antibiotics are done. Also, keep your family's toothbrushes and utensils separate, unless they have been washed.
If repeated cases of strep still occur in a family, check to see if someone is a strep carrier. Carriers have strep in their throats, but the bacteria do not make them sick. Sometimes, treating them can prevent others from getting strep throat.
Alternative Names
Pharyngitis - streptococcal; Streptococcal pharyngitis; Tonsillitis - strep; Sore throat strep
References
Flores AR, Caserta MT. Pharyngitis. In: Bennett JE, Dolin R, Blaser MJ, eds. Mandell, Douglas, and Bennett's Principles and Practice of Infectious Diseases. 9th ed. Philadelphia, PA: Elsevier; 2020:chap 59.
Sur DK, Plesa ML. Antibiotic use in acute upper respiratory tract infections. Am Fam Physician. 2022;106(6):628-636. PMID: 36521460 www.ncbi.nlm.nih.gov/pubmed/36521460/.
Tanz RR. Acute pharyngitis. In: Kliegman RM, St. Geme JW, Blum NJ, Shah SS, Tasker RC, Wilson KM, eds. Nelson Textbook of Pediatrics. 21st ed. Philadelphia, PA: Elsevier; 2020:chap 409.
van Driel ML, De Sutter AI, Thorning S, Christiaens T. Different antibiotic treatments for group A streptococcal pharyngitis. Cochrane Database Syst Rev. 202116;3(3):CD004406. PMID: 33728634 www.ncbi.nlm.nih.gov/pubmed/33728634/.
Review Date 7/8/2023
Updated by: Linda J. Vorvick, MD, Clinical Professor, Department of Family Medicine, UW Medicine, School of Medicine, University of Washington, Seattle, WA. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.