Lactose tolerance tests measure the ability of your intestines to break down a type of sugar called lactose. This sugar is found in milk and other dairy products. If your body cannot break down this sugar, you are said to have lactose intolerance. This can cause gassiness, abdominal pain, cramps, and diarrhea.
How the Test is Performed
Two common methods include:
- Lactose tolerance blood test
- Hydrogen breath test
The hydrogen breath test is the preferred method. It measures the amount of hydrogen in the air you breathe out.
- You will be asked to breathe into a balloon-type container.
- You will then drink a flavored liquid containing lactose.
- Samples of your breath are taken at set times and the hydrogen level is checked.
- Normally, very little hydrogen is in your breath. But if your body has trouble breaking down and absorbing lactose, breath hydrogen levels increase.
The lactose tolerance blood test looks for glucose in your blood. Your body creates glucose when lactose breaks down.
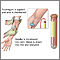
- For this test, several blood samples will be taken before and after you drink a liquid containing lactose.
- A blood sample will be taken from a vein in your arm (venipuncture).
How to Prepare for the Test
You should not eat or do heavy exercise for 8 hours before the test.
How the Test will Feel
There should not be any pain or discomfort when giving a breath sample.
When the needle is inserted to draw blood, some people feel slight pain, while others feel only a prick or stinging feeling. Afterward, there may be some throbbing.
Why the Test is Performed
Your health care provider may order these tests if you have signs of lactose intolerance.
Normal Results
The breath test is considered normal if the increase in hydrogen is less than 20 parts per million (ppm) over your fasting (pre-test) level.
The blood test is considered normal if your glucose level rises more than 30 mg/dL (1.6 mmol/L) within 2 hours of drinking the lactose solution. A rise of 20 to 30 mg/dL (1.1 to 1.6 mmol/L) is inconclusive.
Note: Normal value ranges may vary slightly among different laboratories. Talk to your doctor about the meaning of your specific test results.
The examples above show the common measurements for results for these tests. Some labs use different measurements or may test different samples.
What Abnormal Results Mean
Abnormal results may be a sign of lactose intolerance.
A breath test result that shows a rise in hydrogen content of 20 ppm over your pre-test level is considered a positive test. This means you may have trouble breaking down lactose.
The blood test is considered abnormal if your glucose level rises less than 20 mg/dL (1.1 mmol/L) within 2 hours of drinking the lactose solution.
An abnormal test should be followed by a glucose tolerance test. This will rule out a problem with the body's ability to absorb glucose.
Risks
There is little risk involved with having your blood taken. Veins and arteries vary in size from one person to another and from one side of the body to the other. Taking blood from some people may be more difficult than from others.
Other risks associated with having blood drawn are slight, but may include:
- Fainting or feeling lightheaded
- Multiple punctures to locate veins
- Hematoma (blood buildup under the skin)
- Excessive bleeding
- Infection (a slight risk any time the skin is broken)
Alternative Names
Hydrogen breath test for lactose tolerance
Images
References
Floch MH. Lactose, fructose, and sucrose intolerance. In: Floch MH, ed. Netter's Gastroenterology. 3rd ed. Philadelphia, PA: Elsevier; 2020:chap 63.
Höegenauer C, Hammer HF. Maldigestion and malabsorption. In: Feldman M, Friedman LS, Brandt LJ, eds. Sleisenger and Fordtran's Gastrointestinal and Liver Disease. 11th ed. Philadelphia, PA: Elsevier; 2021:chap 104.
Siddiqi HA, Rabinowitz S, Axiotis CA. Laboratory diagnosis of gastrointestinal and pancreatic disorders. In: McPherson RA, Pincus MR, eds. Henry's Clinical Diagnosis and Management by Laboratory Methods. 24th ed. Philadelphia, PA : Elsevier; 2022:chap 23.
Review Date 7/30/2022
Updated by: Michael M. Phillips, MD, Emeritus Professor of Medicine, The George Washington University School of Medicine, Washington, DC. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.