A food allergy is a type of immune response triggered by eggs, peanuts, milk, shellfish or some other specific food.
Causes
Many people have a food intolerance. This term usually refers to heartburn, cramps, belly pain, or diarrhea that can occur after they eat foods such as:
- Corn products
- Cow's milk and dairy products (usually due to lactose intolerance)
- Wheat and other grains that contain gluten (gluten intolerance or celiac disease)
A true food allergy is much less common.
The immune system normally protects the body against harmful substances, such as bacteria and viruses. It also reacts to foreign substances called allergens. These are usually harmless, and in most people, do not cause a problem.

In a person with a food allergy, the immune response is oversensitive. When it recognizes an allergen, the immune system launches a response. Chemicals such as histamines are released. These chemicals cause allergy symptoms.
Any food can cause an allergic reaction. The most common food allergies are to:
- Eggs (mostly in children)
- Fish (older children and adults)
- Milk (people of all ages)
- Peanuts (people of all ages)
- Shellfish such as shrimp, crab, and lobster (people of all ages)
- Soy (mostly in children)
- Tree nuts (people of all ages)
- Wheat (people of all ages)
In rare cases, food additives, such as dyes, thickeners, or preservatives can cause a food allergy or intolerance reaction.
Some people have an oral allergy. This is an allergy type syndrome that affects the mouth and tongue after they eat certain fresh fruits and vegetables:
- Melons, apples, pineapple, and other foods contain substances that are similar to certain pollens.
- The reaction most often occurs when you eat the raw form of the foods. How severe the reaction is depends on how much of the food you eat.
- Unlike true food allergies, people with the oral allergy syndrome rarely develop severe allergic reactions such as anaphylaxis.
Symptoms
Symptoms usually begin within 2 hours after eating. Sometimes, the symptoms begin a longer time after eating the food.
Key symptoms of a food allergy include hives, a hoarse voice, and wheezing.
Other symptoms that may occur include:
- Swelling (angioedema), especially of the eyelids, face, lips, and tongue
- Trouble swallowing or breathing due to swelling in the throat
- Itching of the mouth, throat, eyes, skin, or any other area
- Lightheadedness or fainting
- Nasal congestion, runny nose
- Stomach cramps, diarrhea, nausea, or vomiting
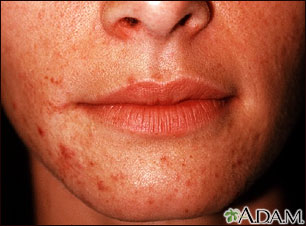
Symptoms of mouth (oral) allergy syndrome:
- Itchy lips, tongue, and throat
- Swollen lips (sometimes)
In a severe reaction, called anaphylaxis, in addition to the above symptoms, you may have low blood pressure and blocked airways. This can be life threatening.
Exams and Tests
Blood or skin tests are sometimes used to confirm that you have an allergy. A double-blind food challenge is one way to diagnose true food allergies. During this test, you and your health care provider will not know what you are eating.
With elimination diets, you avoid the suspected food until your symptoms disappear. Then you start eating the foods again to see if you develop an allergic reaction.
In provocation (challenge) testing, you eat a small amount of the suspected food under medical supervision. This type of test may cause severe allergic reactions. Challenge testing should only be done by a trained provider.
Never try to cause a reaction or reintroduce a food on your own. These tests should only be done under the guidance of a provider, especially if your first reaction was severe.
Treatment
If you suspect that you or your child has a food allergy, see an allergy specialist doctor (allergist).
Treatment may involve any of the following:
- Avoiding the food (this is the most effective treatment).
- Desensitization, during which you eat a small amount of the food each day. This must be done under an allergist's guidance.
Other treatments, including allergy shots and probiotics, have not been proven to help with food allergies.
If your child has a problem with cow's milk formula, your provider may suggest trying a soy-based formula or something called an elemental formula, if it is available.
If you have symptoms on only one area of the body, for example, a hive on the chin after eating the food, you may not need any treatment. The symptoms will likely go away in a brief time. Antihistamines may relieve the discomfort. Soothing skin creams may also provide some relief.
If you have been diagnosed with a food allergy, learn how to use injectable epinephrine. You should have it with you at all times. If you develop any type of serious or whole-body reaction (even hives) after eating the food:
- Inject the epinephrine.
- Then go to the nearest hospital or emergency facility right away, preferably by ambulance.
- If you develop severe allergy symptoms or anaphylaxis, call 911 or the local emergency number.
Support Groups
The following groups can provide more information about food allergies:
- American Academy of Allergy Asthma and Immunology -- www.aaaai.org/Conditions-Treatments/Allergies/Food-Allergy
- Food Allergy Research and Education (FARE) -- www.foodallergy.org/
- National Institute of Allergy and Infectious Diseases -- www.niaid.nih.gov/diseases-conditions/food-allergy
Outlook (Prognosis)
Allergies to peanuts, tree nuts, and shellfish tend to last a lifetime.

Avoiding the problem foods may be easy if the food is uncommon or easy to identify. When eating away from home, ask detailed questions about the food you are served. When buying food, read package ingredients carefully.
Possible Complications
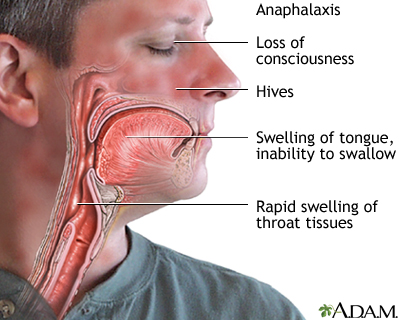
Anaphylaxis is a severe, whole-body allergic reaction that is life threatening. Although people with oral allergy syndrome may have an anaphylactic reaction in rare cases, they should ask their provider if they need to carry injectable epinephrine.
Food allergies can trigger or worsen asthma, eczema, or other disorders.
When to Contact a Medical Professional
Steps to take when a food allergy reaction occurs:
- Call 911 or the local emergency number if you have any serious or whole-body reactions, particularly wheezing or difficulty breathing, after eating any food.
- If your provider prescribed epinephrine for severe reactions, inject it as soon as possible, even before calling 911. The sooner you inject the epinephrine, the better.
- Anyone who has had an allergic reaction to a food should be seen by an allergist.
Prevention
Breastfeeding may help prevent allergies. Otherwise, there is no known way to prevent food allergies.
A common belief and practice is to delay introducing allergy-causing foods to infants until their gastrointestinal tract has had a chance to mature. The timing for this varies from food to food and from baby to baby.
Avoiding peanuts in early childhood does not appear to prevent, and may even enhance, the development of peanut allergy. Providers now suggest introducing peanut-containing foods to infants, which may prevent peanut allergy. Talk to your child's provider to learn more.
Once an allergy has developed, carefully avoiding the offending food usually prevents further problems.
Alternative Names
Allergy to food; Food allergy - peanuts; Food allergy - soy; Food allergy - fish; Food allergy - shellfish; Food allergy - eggs; Food allergy - milk
References
Bird JA, Burks AW. Food allergy. In: Rich RR, Fleisher TA, Schroeder HW, Weyand CM, Corry DB, Puck JM, eds. Clinical Immunology. 6th ed. Philadelphia, PA: Elsevier; 2023:chap 49.
Sicherer SH, Lack G, Jones SM. Food allergy management. In: Burks AW, Holgate ST, O'Hehir RE, et al, eds. Middleton's Allergy: Principles and Practice. 9th ed. Philadelphia, PA: Elsevier; 2020:chap 82.
Togias A, Cooper SF, Acebal ML, et al. Addendum guidelines for the prevention of peanut allergy in the United States: report of the National Institute of Allergy and Infectious Diseases-sponsored expert panel. J Allergy Clin Immunol. 2017;139(1):29-44. PMID: 28065278 pubmed.ncbi.nlm.nih.gov/28065278/.
Test Your Knowledge
Review Date 11/6/2022
Updated by: Stuart I. Henochowicz, MD, FACP, Clinical Professor of Medicine, Division of Allergy, Immunology, and Rheumatology, Georgetown University Medical School, Washington, DC. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.