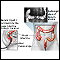
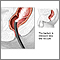
Barium enema is a special x-ray of the large intestine, which includes the colon and rectum.
How the Test is Performed
This test may be done in a health care provider's office or hospital radiology department. It is done after your colon is completely empty and clean. Your provider will give you instructions for cleansing your colon.
During the test:
- You lie flat on your back on the x-ray table. An x-ray is taken.
- You then lie on your side. The provider gently inserts a well-lubricated tube (enema tube) into your rectum. The tube is connected to a bag that holds a liquid containing barium sulfate. This is a contrast material that highlights specific areas in the colon, creating a clear image.
- The barium flows into your colon. X-rays are taken. A small balloon at the tip of the enema tube may be inflated to help keep the barium inside your colon. The provider monitors the flow of the barium on an x-ray screen.
- Sometimes a small amount of air is delivered into the colon to expand it. This allows for even clearer images. This test is called a double contrast barium enema.
- You are asked to move into different positions. The table will move up and down to get different views. At certain times when the x-ray pictures are taken, you are told to hold your breath and be still for a few seconds so the images will not be blurry.
- The enema tube is removed after the x-rays are taken.
- You are then given a bedpan or helped to the toilet, so you can empty your bowels and remove as much of the barium as possible. Afterward, 1 or 2 more x-rays may be taken.
How to Prepare for the Test
Your bowels need to be completely empty for the exam. If they are not empty, the test may miss a problem in your large intestine.
You will be given instructions for cleansing your bowel using an enema or laxatives. This is also called bowel preparation. Follow the instructions exactly.
For 1 to 3 days before the test, you need to be on a clear liquid diet. Examples of clear liquids are:
- Clear coffee or tea
- Fat-free bouillon or broth
- Gelatin
- Sports drinks
- Strained fruit juices
- Water
How the Test will Feel
When barium enters your colon, you may feel like you need to have a bowel movement. You may also have:
- A feeling of fullness
- Moderate to severe cramping
- General discomfort
Taking long, deep breaths may help you relax during the procedure.
It is normal for your stools to be white for a few days after this test. Drink extra fluids for 2 to 4 days. Ask your provider about a laxative if you develop hard stools.
Why the Test is Performed
The barium enema test is used to:
- Detect or screen for colon cancer
- Diagnose or monitor ulcerative colitis or Crohn disease
- Diagnose the cause of blood in stools, diarrhea, or very hard stools (constipation)
The barium enema test is used much less often than in the past. Colonoscopy is done more often now. Another alternative, CT colonography, has been used as well.
Normal Results
Barium should fill the colon evenly, showing normal bowel shape and position and no blockages.
What Abnormal Results Mean
Abnormal test results may be a sign of:
- Blockage of the large intestine
- Narrowing of the colon above the rectum (Hirschsprung disease in infants)
- Crohn disease or ulcerative colitis
- Cancer in the colon or rectum
- Sliding of one part of the intestine into another (intussusception)
- Small growths that stick out of the lining of the colon, called polyps
- Small, bulging sacs or pouches of the inner lining of the intestine, called diverticula
- Twisted loop of the bowel (volvulus)
Risks
There is low radiation exposure. X-rays are monitored so that the smallest amount of radiation is used. Pregnant women and children are more sensitive to x-ray risks.
Alternative Names
Lower gastrointestinal series; Lower GI series; Colorectal cancer - lower GI series; Colorectal cancer - barium enema; Crohn disease - lower GI series; Crohn disease - barium enema; Intestinal blockage - lower GI series; Intestinal blockage - barium enema
References
Boone D, Plumb A, Taylor SA. The large bowel. In: Adam A, Dixon AK, Gillard JH, Schaefer-Prokop CM, eds. Grainger & Allison's Diagnostic Radiology. 7th ed. Philadelphia, PA: Elsevier; 2021:chap 22.
Rubesin SE. Barium studies of the small bowel. In: Gore RM, ed. Textbook of Gastrointestinal Radiology. 5th ed. Philadelphia, PA: Elsevier; 2022:chap 24.
US Preventive Services Task Force website. Final recommendation statement. Colorectal cancer: screening. www.uspreventiveservicestaskforce.org/uspstf/recommendation/colorectal-cancer-screening. Published May 18, 2021. Accessed February 3, 2024.
Review Date 1/7/2023
Updated by: Jason Levy, MD, FSIR, Northside Radiology Associates, Atlanta, GA. Internal review and update on 02/03/2024 by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.