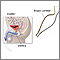
Bladder biopsy is a procedure in which small pieces of tissue are removed from the bladder. The tissue is tested under a microscope.
How the Test is Performed
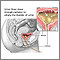
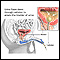
A bladder biopsy can be done as part of a cystoscopy. Cystoscopy is a procedure that is done to see the inside of the bladder using a thin lighted tube called a cystoscope. A small piece of tissue or the entire abnormal area is removed. The tissue is sent to the lab to be tested if:
- Abnormalities of the bladder are found during this exam
- A tumor is seen
How to Prepare for the Test
You must sign an informed consent form before you have a bladder biopsy. In most cases, you are asked to urinate just before the procedure. You may also be asked to take an antibiotic before the procedure.
For infants and children, the preparation you can provide for this test depends on your child's age, previous experiences, and level of trust. For general information regarding how you can prepare your child, see the following topics:
- Infant test or procedure preparation (birth to 1 year)
- Toddler test or procedure preparation (1 to 3 years)
- Preschooler test or procedure preparation (3 to 6 years)
- School age test or procedure preparation (6 to 12 years)
- Adolescent test or procedure preparation (12 to 18 years)
How the Test will Feel
You may have a slight discomfort as the cystoscope is passed through your urethra into your bladder. You will feel discomfort that is similar to a strong urge to urinate when the fluid has filled your bladder.
You may feel a pinch during the biopsy. There may be a burning sensation when the blood vessels are sealed to stop bleeding (cauterized).
After the cystoscope is removed, your urethra may be sore. You may feel a burning sensation during urination for a day or two. There may be blood in the urine. In most cases, this will go away on its own.
In some cases, the biopsy needs to be taken from a large area. In that case, you may need general anesthesia or sedation before the procedure.
Why the Test is Performed
This test is most often done to check for cancer of the bladder or urethra.
What Abnormal Results Mean
The presence of cancer cells indicates bladder cancer. The type of cancer can be determined from the biopsy sample.
Other abnormalities may include:
- Bladder diverticula
- Cysts
- Inflammation
- Infection
- Ulcers
Risks
There is some risk for urinary tract infection (UTI).
There is a slight risk for excessive bleeding. There may be a rupture of the bladder wall with the cystoscope or during biopsy.
There is also a risk that the biopsy will fail to detect a serious condition.
Considerations
You will likely have a small amount of blood in your urine shortly after this procedure. If the bleeding continues after you urinate, contact your health care provider.
Also contact your provider if:
- You have pain, chills, or a fever
- You are producing less urine than usual (oliguria)
- You cannot urinate despite a strong urge to do so
Alternative Names
Biopsy - bladder
References
Cundiff GW, Bent AE. Cystourethroscopy. In: Baggish MS, Karram MM, eds. Atlas of Pelvic Anatomy and Gynecologic Surgery. 5th ed. Philadelphia, PA: Elsevier; 2021:chap 120.
Duty BD, Conlin MJ. Principles of urologic endoscopy. In: Partin AW, Dmochowski RR, Kavoussi LR, Peters CA, eds. Campbell-Walsh-Wein Urology. 12th ed. Philadelphia, PA: Elsevier; 2021:chap 13.
National Institute of Diabetes and Digestive and Kidney Diseases website. Cystoscopy and ureteroscopy. www.niddk.nih.gov/health-information/diagnostic-tests/cystoscopy-ureteroscopy. Updated July 2021. Accessed August 23, 2022.
Taylor JM, Smith TG, Coburn M. Urologic surgery. In: Townsend CM Jr, Beauchamp RD, Evers BM, Mattox KL, eds. Sabiston Textbook of Surgery. 21st ed. Philadelphia, PA: Elsevier; 2022:chap 74.
Review Date 4/10/2022
Updated by: Kelly L. Stratton, MD, FACS, Associate Professor, Department of Urology, University of Oklahoma Health Sciences Center, Oklahoma City, OK. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.