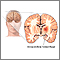
You were in the hospital after having a stroke. Stroke happens when blood flow to part of the brain stops.
At home follow your health care provider's instructions on self-care. Use the information below as a reminder.
When You're in the Hospital
First, you received treatment to prevent further damage to the brain, and to help the heart, lungs, and other important organs heal.
After you were stable, doctors did testing and started treatment to help you recover from the stroke and prevent a future stroke. You may have stayed in a special unit that helps people recover after a stroke.
What to Expect at Home
Because of possible injury to the brain from the stroke, you may notice problems with:
- Changes in behavior
- Doing easy tasks
- Memory
- Moving one side of the body
- Muscle spasms
- Paying attention
- Sensation or awareness of one part of the body
- Swallowing
- Talking or understanding others
- Thinking
- Seeing to one side (hemianopia)
You may need help with daily activities you used to do alone before the stroke.
Depression after a stroke is fairly common as you learn to live with the changes. It may develop soon after the stroke or up to 2 years after the stroke.
Do not drive your car without your provider's permission.
Moving Around
Moving around and doing normal tasks may be hard after a stroke.
Make sure your home is safe. Ask your provider, therapist, or nurse about making changes in your home to make it easier to do everyday activities.
Find out about what you can do to prevent falls and keep your bathroom safe to use.
Family and caregivers may need to help with:
- Exercises to keep your elbows, shoulders, and other joints loose
- Watching for joint tightening (contractures)
- Making sure splints are used in the correct way
- Making sure arms and legs are in a good position when sitting or lying
If you or your loved one is using a wheelchair, follow-up visits to make sure it fits well are important to prevent skin ulcers.
- Check every day for pressure sores at the heels, ankles, knees, hips, tailbone, and elbows.
- Change positions in the wheelchair several times per hour during the day to prevent pressure ulcers.
- If you have problems with spasticity, learn what makes it worse. You or your caregiver can learn exercises to keep your muscles loose.
- Learn how to prevent pressure ulcers.
Thinking and Speaking
Tips for making clothing easier to put on and take off are:
- Velcro is much easier than buttons and zippers. All buttons and zippers should be on the front of a piece of clothing.
- Use pullover clothes and slip-on shoes.
People who have had a stroke may have speech or language problems. Tips for family and caregivers to improve communication include:
- Keep distractions and noise down. Keep your voice lower. Move to a quieter room. Do not shout.
- Allow plenty of time for the person to answer questions and understand instructions. After a stroke, it takes longer to process what has been said.
- Use simple words and sentences, speak slowly. Ask questions in a way that can be answered with a yes or no. When possible, give clear choices. Do not give too many options.
- Break down instructions into small and simple steps.
- Repeat if needed. Use familiar names and places. Announce when you are going to change the subject.
- Make eye contact before touching or speaking if possible.
- Use props or visual prompts when possible. Do not give too many options. You may be able to use pointing or hand gestures or drawings. Use an electronic device, such as a tablet computer or cell phone, to show pictures to help with communication.
Bowel Care
Nerves that help the bowels work smoothly can be damaged after a stroke. Have a routine. Once you find a bowel routine that works, stick to it:
- Pick a regular time, such as after a meal or a warm bath, to try to have a bowel movement.
- Be patient. It may take 15 to 45 minutes to have bowel movements.
- Try gently rubbing your stomach to help stool move through your colon.
Avoid constipation:
- Drink more fluids.
- Stay active or become more active as much as possible.
- Eat foods with lots of fiber.
Ask your provider about medicines you are taking that may cause constipation (such as medicines for depression, pain, bladder control, and muscle spasms).
Tips for Taking Medicines
Have all of your prescriptions filled before you go home. It is very important that you take your medicines the way your provider told you to. Do not take any other drugs, supplements, vitamins, or herbs without asking your provider about them first.
You may be given one or more of the following medicines. These are meant to control your blood pressure or cholesterol, and to keep your blood from clotting. They may help prevent another stroke:
- Antiplatelet medicines (aspirin or clopidogrel) help keep your blood from clotting.
- Beta blockers, diuretics (water pills), and ACE inhibitor medicines control your blood pressure and protect your heart.
- Statins lower your cholesterol.
- If you have diabetes, control your blood sugar at the level your provider recommends.
Do not stop taking any of these medicines.
If you are taking a blood thinner, such as warfarin (Coumadin), you may need to have extra blood tests done.
Staying Healthy
If you have problems with swallowing, you must learn to follow a special diet that makes eating safer. The signs of swallowing problems are choking or coughing when eating. Learn tips to make feeding and swallowing easier and safer.
Avoid salty and fatty foods and stay away from fast food restaurants to make your heart and blood vessels healthier.
Limit how much alcohol you drink to a maximum of 1 drink a day if you are a woman and 2 drinks a day if you are a man. Ask your provider if it is OK for you to drink alcohol.
Keep up to date with your vaccinations. Get a flu shot every year. Ask your provider if you need a vaccination to prevent pneumococcal infections (sometimes called a "pneumonia shot").
Do not smoke. Ask your provider for help quitting if you need to. Do not let anybody smoke in your home.
Try to stay away from stressful situations. If you feel stressed all the time or feel very sad, talk with your provider.
If you feel sad or depressed at times, talk to family or friends about this. Ask your provider about seeking professional help.
When to Call the Doctor
Contact your provider if you have:
- Problems taking medicines for muscle spasms
- Problems moving your joints (joint contracture)
- Problems moving around or getting out of your bed or chair
- Skin sores or redness
- Pain that is becoming worse
- Recent falls
- Choking or coughing when eating
- Signs of a bladder infection (fever, burning when you urinate, or frequent urination)
Call 911 or the local emergency number if the following symptoms develop suddenly or are new:
- Numbness or weakness of the face, arm, or leg
- Blurry or decreased vision
- Not able to speak or understand
- Dizziness, loss of balance, or falling
- Severe headache
Alternative Names
Cerebrovascular disease - discharge; CVA - discharge; Cerebral infarction - discharge; Cerebral hemorrhage - discharge; Ischemic stroke - discharge; Stroke - ischemic - discharge; Stroke secondary to atrial fibrillation - discharge; Cardioembolic stroke - discharge; Brain bleeding - discharge; Brain hemorrhage - discharge; Stroke - hemorrhagic - discharge; Hemorrhagic cerebrovascular disease - discharge; Cerebrovascular accident - discharge
Images
References
Dobkin BH. Rehabilitation and recovery of the patient with stroke. In: Grotta JC, Albers GW, Broderick JP, et al, eds. Stroke: Pathophysiology, Diagnosis, and Management. 7th ed. Philadelphia, PA: Elsevier; 2022:chap 60.
Kernan WN, Ovbiagele B, Black HR, et al. Guidelines for the prevention of stroke in patients with stroke and transient ischemic attack: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. 2014;45(7):2160-2236. PMID: 24788967 pubmed.ncbi.nlm.nih.gov/24788967/.
National Institutes of Health. National Institute of Neurological Disorders and Stroke website. Post-stroke rehabilitation fact sheet. www.ninds.nih.gov/post-stroke-rehabilitation-fact-sheet. Updated July 25, 2022. Accessed September 29, 2022.
Winstein CJ, Stein J, Arena R, et al. Guidelines for adult stroke rehabilitation and recovery: a guideline for healthcare professionals from the American Heart Association/American Stroke Association. Stroke. 2016;47(6):e98-e169. PMID: 27145936 pubmed.ncbi.nlm.nih.gov/27145936/.
Patient Instructions
- ACE inhibitors
- Antiplatelet drugs - P2Y12 inhibitors
- Aspirin and heart disease
- Bathroom safety for adults
- Brain surgery - discharge
- Butter, margarine, and cooking oils
- Caring for muscle spasticity or spasms
- Cholesterol and lifestyle
- Cholesterol - drug treatment
- Communicating with someone with aphasia
- Communicating with someone with dysarthria
- Constipation - self-care
- Constipation - what to ask your doctor
- Controlling your high blood pressure
- Daily bowel care program
- Dementia and driving
- Dementia - behavior and sleep problems
- Dementia - daily care
- Dementia - keeping safe in the home
- Dementia - what to ask your doctor
- Dietary fats explained
- Fast food tips
- Gastrostomy feeding tube - bolus
- Jejunostomy feeding tube
- Kegel exercises - self-care
- Low-salt diet
- Mediterranean diet
- Pressure ulcers - what to ask your doctor
- Preventing falls
- Preventing falls - what to ask your doctor
- Preventing pressure ulcers
- Self catheterization - female
- Self catheterization - male
- Suprapubic catheter care
- Swallowing problems
- Urine drainage bags
- When you have urinary incontinence
Review Date 7/26/2022
Updated by: Evelyn O. Berman, MD, Assistant Professor of Neurology and Pediatrics at University of Rochester, Rochester, NY. Review provided by VeriMed Healthcare Network. Also reviewed by David C. Dugdale, MD, Medical Director, Brenda Conaway, Editorial Director, and the A.D.A.M. Editorial team.