Mental Health and Drug Abuse
Mental Health and Drug Abuse
The problems of alcohol and drug abuse and mental health are being studied in three research institutes now part of the National Institutes of Health (NIH) as well as in the Substance Abuse and Mental Health Services Administration (SAMHSA). The NIH research institutes are the National Institute on Alcohol Abuse and Alcoholism, the National Institute on Drug Abuse, and the National Institute of Mental Health.
Federal involvement with mental health goes back to the mid 19th century when St. Elizabeths Hospital for the mentally ill opened in Washington. D.C. But it was only in the second decade of this century that the Public Health Service began systematic field studies related to mental health, focusing on school children. A Division of Mental Hygiene was established in the Public Health Service in 1930 and became the National Institute of Mental Health in 1949.
The importance of the problem of drug addiction was also recognized by the Federal Government in the 1920s and 1930s, and two hospitals for the treatment of narcotic addicts were created within the Service.
Concern with these problems continues in the work of the three institutes and SAMHSA. They provide financial support for a broad spectrum of basic, applied, and clinical research, ranging from investigations at the molecular level to study of risk factors in the environment. Prevention projects, dissemination of scientific and technical information, and the provision of professional and technical assistance to states and communities in operating alcohol, drug abuse, and mental health programs are also important objectives.
Gallery
A chemistry laboratory in St. Elizabeths Hospital's Blackburn Laboratory of Pathology. When St. Elizabeths, the first national mental hospital in the United States, opened in 1855, very little was known about the causes of mental disease. Thus, in 1884, Superintendent W.W. Godding appointed pathologist Isaac W. Blackburn, a pioneer in neuropathology, as chief of the first pathology laboratory established in a mental hospital in this country, and charged him with the task of studying the pathology of mental disease.
c. 1910
In order to understand better the pathology of mental disease a very rich collection of pathologic material was gathered together over the past century at the Blackburn Laboratory of Pathology at Saint Elizabeths Hospital. This drawing of an endothelial sarcoma of the dura mater (inner lining of the brain and spinal cord) was made by portrait artist and neurologist Isaac Blackburn, the first chief of the pathology laboratory. Numerous reports of neuropathologic changes in patients who died with a variety of nervous and mental diseases in the hospital were published by researchers at the Blackburn Laboratory.
c. 1895
A nurse at St. Elizabeths Hospital for the mentally ill in Washington, D.C., monitors patients in continuously flowing baths which were supposed to have a soothing effect on the nerves. Cold packs can also be seen on the heads of patients. Hydrotherapy was one of the innovations at St. Elizabeths which began using it in 1897. Many other types of therapies were also tried, ranging from "moral treatment" in the 19th century that provided congenial, homelike surroundings in which mentally ill patients could learn from the example of healthy attendants to psychoanalysis in the 20th century.
c. 1950
Art therapy has been a part of the treatment program for psychiatric patients at St. Elizabeths Hospital since 1924 when Dr. Nolan Lewis argued for the value of art in expressing the unconscious and projecting inner feelings. In the 1940s and 1950s, Prentiss Taylor was the first art therapist to work as a regular member of the hospital staff. He published on art as psychotherapy and put together a large traveling exhibition of patients' works. Here, Dr. John Lind, who treated the criminally insane, displays the handiwork of one of his patients entitled "dimensional divertissement."
c. 1950
Dr. Adam Metheny gives psychometric tests to a child in the Mental Retardation Clinic of the National Institute of Child Health and Human Development (NICHD). Much of the work at the NICHD in the 1980s has shifted to the molecular level. Scientists study development in animal models in order to understand human development better, especially the mechanism of cell differentiation. Errors in this process not only produce birth defects that can lead to mental retardation, but also set the stage for diseases such as cancer, premature aging, and immune disorders.
1975
Scientists at the National Institute of Mental Health and other research institutions in the Public Health Service dealing with mental illness have experimented with many different kinds of treatment methods. Here, psychiatrist Dr. Milton Shore uses puppets in his work with child patients.
c. 1970
Among a number of important clinical studies, intramural scientists at the National Institute on Alcohol Abuse and Alcoholism are studying the special problems of the homeless alcoholic.
c. 1980
The view of alcoholism as a single disorder arising from purely environmental causes or the result of "moral" weakness has been changing rapidly in light of recent evidence concerning genetic factors that predispose the development of alcoholism. Working with animal models of alcohol tolerance and dependence, intramural scientists of the National Institute on Alcohol Abuse and Alcoholism have been able to investigate the addictive process at the cellular and subcellular levels. Clinical studies using recently developed classifications of alcoholics are beginning to yield results about the differing contributions of environmental and biologic factors.
c. 1980
In 1929, feeling that drug addiction was primarily a medical and social problem and that treatment of addiction by incarceration in prisons was illogical, Congress passed a law establishing two United States "narcotic farms" for the confinement and treatment of persons addicted to the use of habit-forming narcotic drugs. The first of these "farms," whose name was later changed to U.S. Public Health Service Hospital, is pictured here. It was built at Lexington, Kentucky, and opened to patients in 1935. The second was established at Forth Worth, Texas, and was opened in 1938.
c. 1950
Scientists at the Lexington Hospital began mapping the brain to learn the effects of many abused substances and the causes of addiction. Drugs studied range from the opiates and barbiturates to nicotine and cocaine. The Addiction Research Center neuroscientists are continuing this pioneering work to identify receptor sites in the nervous system for all types of psychoactive drugs. The work includes basic molecular studies, preclinical work with animals, and clinical studies with human volunteers.
c. 1965
The program of treatment at the Lexington Hospital included the withdrawal of drugs, the rehabilitation of the addict, and assistance to the patient in finding employment following discharge from the hospital. The rehabilitation program consisted of medical treatment for any correctable physical defects, vocational therapy designed to maintain or add to skills which the addict already possessed, and psychotherapy in selected cases.
c. 1965
The research unit at the Lexington Hospital, later named the Addiction Research Center, studied the nature of the addictive process and searched for a nonaddicting painkiller as an alternative to morphine. From this research emerged methods for determining the abuse potential of new psychoactive drugs that are proposed for therapeutic use. Tracking how and where drugs exert their actions in the central nervous system, especially the brain, in order to understand how psychoactive drugs produce their rewarding effects was another aspect of their work.
c. 1965
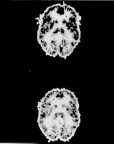
The Addiction Research Center (ARC) became part of the National Institute on Drug Abuse when it was created in 1973 and moved from Lexington to Baltimore, Maryland, in 1979. The ARC has become the largest facility in the United States devoted to studying addiction and drug abuse. Researchers at the ARC in Baltimore use new noninvasive imaging techniques, such as positron emission tomography (PET scanning), to produce images of the sites of action of drugs in the living human brain. The PET scan below, taken from a former opioid addict under the influence of morphine, shows decreased brain activity (lighter tones) as compared to activity in the same brain under the placebo (no drug) above.
c. 1980